2025-12-17T17:11:43
Why OBGYN Clinics Are Using Nitrous Oxide for Pain Relief
- OB/GYN

March 14, 2017 | OB/GYN
Specialties:OB/GYN
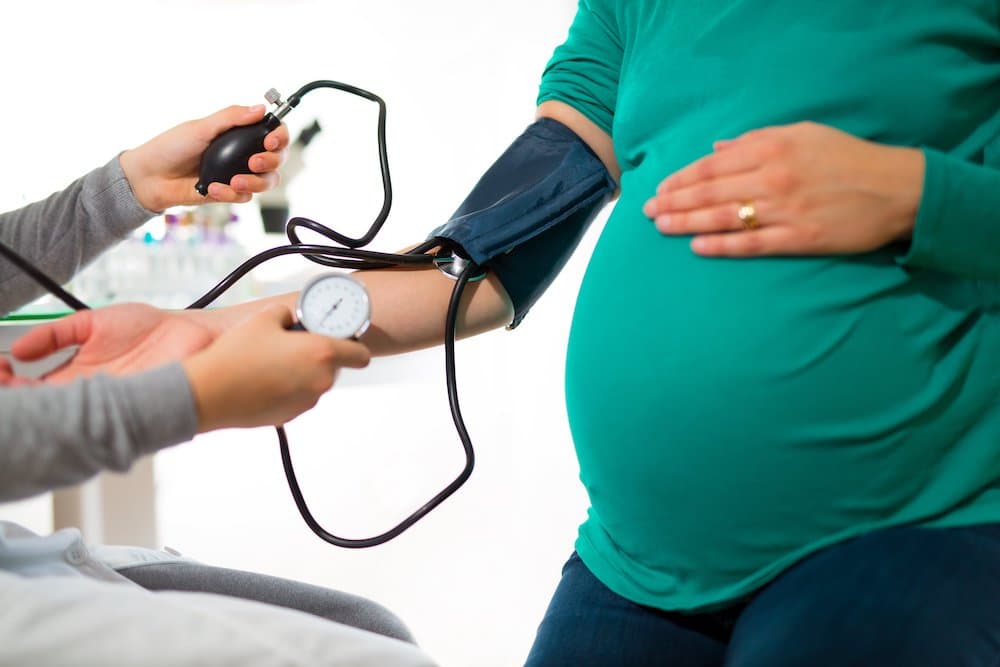
A number of different conditions can affect pregnant women, especially in the later stages of pregnancy. Regular checkups and monitoring is important during pregnancy, as this can help detect and prevent many of these conditions before they become serious and put the mother or baby at risk.
One of these conditions is known as preeclampsia, a complication that is characterized by high blood pressure and indications of damage to other organs, like the kidneys. Preeclampsia is the earlier stage of eclampsia, a serious condition that can negatively affect both the mother and baby.
Most cases of preeclampsia are noticeable at around 20 weeks of pregnancy, and it requires immediate medical attention. If not treated right away, preeclampsia can lead to additional complications.
Doctors have not yet found any exact causes of preeclampsia. However, they are certain of a few things:
Preeclampsia affects functions of the placenta, which provides nutrients for the fetus during the pregnancy. The placenta receives blood from new blood vessels that develop in pregnancy, but in cases of preeclampsia, this process doesn’t happen correctly. Usually, this occurs because the blood vessels don’t develop properly, e.g., they are too narrow, don’t respond the right way to hormone signals, etc. There are a few known causes of this unusual blood vessel development including:
Though there aren’t any definite causes, there are several factors that have been known to raise the risk of preeclampsia for pregnant women such as:
Symptoms of preeclampsia aren’t always noticeable. However, blood pressure is often the most common sign—even a small increase from the recommended 140/90 threshold can be a sign of the disease.
Other symptoms can include:
Because some of these factors might signify other conditions, particularly weight gain and swelling, doctors usually look for a presence of multiple symptoms to make a diagnosis—usually high blood pressure and another symptom.
If it’s not treated the right way, and promptly, preeclampsia can lead to several complications:
Diagnosis of preeclampsia requires the presence of high blood pressure and one or more of the symptoms listed above. There are other conditions that high blood pressure might indicate, so your doctor will have to rule those out. A few extra tests that might be needed to confirm preeclampsia include:
During pregnancy, there is only one cure for preeclampsia: delivery. However, depending on the severity, there are ways it can be managed without an early delivery, which may put the baby and mother at risk. Your doctor will look at several factors when deciding if you need to deliver right away. If you don’t, treatment can include:
Unfortunately, there are limited proven ways to prevent preeclampsia. There are only two medications that have shown a reduced risk in some cases:
In general, doctors recommend staying as healthy as you can both before and during pregnancy. If you are at risk for preeclampsia or are demonstrating symptoms, don’t wait—prompt treatment can make a big difference, so be sure to speak to your doctor right away.
“Preeclampsia.” The Mayo Clinic. http://www.mayoclinic.org/diseases-conditions/preeclampsia/basics/definition/con-20031644
“Preeclampsia and Eclampsia.” WebMD. http://www.webmd.com/baby/guide/preeclampsia-eclampsia#1
WRITTEN BY:
OB/GYN

2025-12-17T17:11:43

2025-11-21T14:10:25

2024-09-19T11:59:35

2019-12-31T15:15:01
This information is not intended to replace the advice of a medical professional. You should always consult your doctor before making decisions about your health.